Menstuff® has compiled the following information on the Human
Papillomavirus Virus. 60% and 80% of women diagnosed with cervical
cancer have not had a pap smear in the past 5 years! E-Mail
for help or visit their HPV
Chat Room ![]() weekdays from 5pm-6pm, ET. Men - See how to prevent
getting genital warts.
weekdays from 5pm-6pm, ET. Men - See how to prevent
getting genital warts.
Get a free subscription to HPV Today. Log in to
www.hpvtoday.com
![]() and choose ESTADOS UNIDOS
and choose ESTADOS UNIDOS
Related issues: Talking
With Kids About Tough Issues AIDS,
Bacterial Vaginosis, Blue
Balls, Chancroid, Chlamydia,
Condoms, Contraception,
Crabs, Genital
Herpes, Genital Warts, Gonorrhea,
Hepatitis A,
B, C,
D, E,
Impotency, Nongonococcal
Urethritis, Pelvic Inflammatory Disease,
Reproduction, STDS,
Syphilis, Trichomoniasis,
Yeast Infection
Does HPV vaccination affect teens’
sexual behavior?
Published in CMAJ, the findings by Canadian investigators are from an analysis of data from nearly 300,000 heterosexual girls. The information was collected on the BC Adolescent Health Survey, a longitudinal provincial survey administered in schools to capture adolescent physical and emotional health indicators. Using linear trend analysis, the researchers looked at sexual health behaviors and risk factors in adolescent girls before and after the implementation of HPV vaccination (2003, 2008, and 2013).
Conducted every 5 or 6 years since 1992, the BC Adolescent Health Survey represents more than 1.4 million students in grades 7 through 12 in public schools in British Columbia (BC). The survey is anonymous and does not capture identifiable data. In addition to demographics, information is collected on ever having sexual intercourse, age at first intercourse and number of sexual partners in the last year. In relation to last intercourse, the students also are asked about substance, birth control and condom use, and whether they have ever been pregnant.
The researchers found that from 2003 to 2013, the proportion of girls ever having intercourse decreased from 21.3% to 18.3%; adjusted odds ratio (OR) 0.79. From 2008 to 2013, self-reports of sexual intercourse before age 14 decreased significantly (adjusted OR 0.76) as did reported substance use before intercourse (adjusted OR 0.69 for 2003-2013). From 2003 to 2013, there was no significant change in number of sexual partners reported. After implementation of the HPV vaccination program, condom use significantly increased (adjusted OR 1.19, 95% confidence interval [CI] 1.02-1.39) and prevalence of girls reporting pregnancy decreased by 42% (adjusted OR 0.56, 95% CI 0.40-0.80).
The authors said that because of its large sample size and complex sampling technique coupled with a high rate of response to the survey, the study is representative of the BC population. It is limited in that the researchers did not look at the direct relationship between individual HPV vaccination status and sexual behaviors. Also, individual-level or causal relationships cannot be inferred because no identifiable data were captured that could be linked to public health vaccination records.
“Future analyses,” the authors said in conclusion,
“should explore differences between girls who identify with
other sexual orientations such as homosexuality and evaluate sexual
behavior among girls who received the HPV vaccine and those who did
not.”
Source: www.contemporaryobgyn.net/hpv/does-hpv-vaccination-affect-teens-sexual-behavior
Men - Have you had your HPV vaccine
shot?
(Editor's warning: There is too much evidence that Merck's vaccine Gardasil is detrimental to girls health and should not be given.)
The ACIP recommendation is limited to Gardasil®, one of two FDA-approved HPV vaccines. The three-dose immunization has been found to be safe and effective in protecting males from contracting genital warts.
However, while the ACIP believes males can benefit from HPV vaccination, it did not advise routine vacation for boys and young men, as it has for girls and young women. As the committee stated, “Because the health burden is greater in females than males, and numerous models have shown vaccination of adolescent girls to be a cost-effective use of public health resources, improving coverage in females aged 11 and 12 years could potentially be a more effective and cost-effective strategy than adding male vaccination.”
While HPV vaccination may be effective, results from a new
national survey of men aged 18–59 in the United States indicate
both low knowledge about HPV among surveyed men and only moderate HPV
vaccine acceptability, with just over one-third of participants (37%)
stating they would be willing to get HPV vaccine. Results of the
survey were recently published in the journal Sexually Transmitted
Infections.
Background Information
Human papillomavirus (HPV) is a sexually transmitted disease that
is highly prevalent, yet often misunderstood. Recent scientific
advances have established that certain types of HPV can cause
cervical cancer. However, this cancer can almost always be prevented
through regular screening and, if needed, treatment of abnormal cell
changes. The challenge is to provide focused, much-needed education
about HPV without causing undue fear.
Approximately 5.5 million new cases of sexually transmitted HPV occur in the U.S. each year, with at least 20 million people estimated to be currently infected. Direct annual medical costs for treating symptoms of HPV infection in the United States are estimated at $1.6 billion and the cost of the cervical cancer screening program (Pap smears) is $5 billion - $6 billion every year. Because research linking genital HPV and cervical cancer is relatively new, there is considerable confusion among patients, medical professionals, policy makers and the general public as to the best counseling, screening, treatment and prevention practices. Additionally, while anal and penile cancers are uncommon, HPV can put men at risk for these cancers, so care should be taken not to leave them out of these equations.
The majority of Americans are unaware of the link between certain types of HPV and cervical cancer: in one national survey, 70 percent of women were unable to name the cause of cervical cancer, and 76 percent had never heard of HPV. Additionally, fewer than half of clinicians responding to a Centers for Disease Control and Prevention (CDC) survey in 2004 were aware of differences between "high-risk" and "low-risk" HPV types. Exciting new technologies and research findings have advanced the capacity to conduct better HPV and cervical cancer screening, diagnosis, and treatment. Yet, their role in clinical management is often misunderstood.
This lack of clarity, coupled with discomfort surrounding issues related to STDs and limited provider time for counseling/patient education, contribute to what is often perceived by patients as inadequate and inconsistent information and advice. Misinformation and overly frightening views about genital HPV abound. Many patients are puzzled or angry that they were unaware of HPV and their personal risk for acquiring the virus. Many are frustrated by the difficulty of finding clear, accurate, up-to-date information and counseling about a potentially life-threatening condition.
Among policy makers, the misinformation and confusion surrounding HPV has fueled discussion. In 1999, Congress debated whether to require screening and reporting for HPV, condom labeling, and warnings on educational materials about HPV and other STDs. Overall, federal funding in HPV research and treatment is limited in scope and remains poorly funded.
There is a clear public health need for ASHA's National HPV &
Cervical Cancer Prevention Resource Center to serve as a
comprehensive resource for the public, patients, providers, and
policy makers. Increased awareness about HPV and cervical cancer
prevention will reduce unnecessary deaths from this preventable
cancer.
HPV Vaccine
for Your Daughter
Parents should demand full answers about this vaccine's use (high
effectiveness in the 27-month study, but no long-range studies have
been done), just as they do any other health procedure. But,
regardless of whether you'd support mandated or optional vaccines,
use this
issue as a teachable moment for you and your daughter. She
needs to know that sexually transmitted diseases and infections are a
reality for millions of girls and boys. Honest discussion of all the
possible side effects of sexual activity - from pregnancy to STDs and
relationship issues - is the best way to prevent, not cause, physical
and emotional harm from early sexual activity. (Related issue:
Abstinance Failure.)
General STD information is accessible via www.iwannaknow.org
for teens.
The emotional toll of dealing with HPV is often as difficult as the medical aspects and can be more awkward to address. This may be the area where you feel most vulnerable, and the lack of clear counseling messages can make this even more stressful, especially where relationships are concerned.
We regularly receive questions about what to tell either a current
or future sex partner about HPV, for example. The better educated you
are about HPV, the easier it is to give partners the information
needed to answer common questions. Use the information in this
section (and elsewhere on ASHA’s Web site) to give yourself a
good foundation of knowledge.
Prior to discussing things with a partner think about addressing any of your own questions or issues about HPV. This is to help establish your own comfort level and is where knowledge really does equal power. One of the most important aspects of coping with HPV, and helping partners develop a good understanding of the virus, is getting factual information and avoiding myths and hype.
It may also be a good idea to have resources to which you can direct a partner, so you know they turn to trustworthy sources for information. In addition to this information, see our links page for more sites with HPV information
First, remember that having HPV does not mean you have done anything wrong. As mentioned above, most sexually active people are likely to be exposed to HPV at some point, though most never have visible symptoms and remain unaware. Having HPV simply means you, like so many others, have been exposed to a common virus. It is not a reflection on you, your character, or your values, and conversations with partners should not be viewed as making a “confession” or offering an “apology”.
With a new relationship it may be good to date for awhile and allow aspects of the relationship besides sex to develop as you get to know one another and become closer.
HPV types:
There are over 100 types of HPV, about 30 of which are primarily associated with anogenital skin and sexual transmission. Of these types, some can cause genital warts (“low-risk” HPV) while others may cause abnormal cell changes, most commonly of the cervix (“high-risk” HPV).
HPV Latency:
It can take weeks, months, or even years after exposure to HPV before symptoms develop or the virus is detected. This is why it is usually impossible to determine when or from whom HPV may have been contracted.
A recent diagnosis of HPV does not necessarily mean anyone has been unfaithful, even in a long-term relationship spanning years.
Medical Impact:
The medical risks of genital HPV do exist and should not to be overlooked, but a key point is that for most people, HPV is a harmless infection that does not result in visible symptoms or health complications.
Very few cases of “high-risk” HPV will lead to cervical cancer, for example, primarily because the immune response is usually able to suppress the virus before cancer develops. In some cases, HPV may cause cell changes that persist for years, and the cells can eventually become cancerous if not detected in time. However, regular screening (such as Pap tests) can almost always find abnormalities so they can be treated, if needed, before cancer occurs.
Some other cancers associated with “high-risk” HPV
include those of the anus, penis, vagina, and vulva. These cancers
are not common and are very rare in industrialized nations,
however.
Most sexually active couples share HPV until the immune response
suppresses the infection. Partners who are sexually intimate only
with each other are not likely to pass the same virus back and forth.
When HPV infection goes away the immune system will remember that HPV
type and keep a new infection of the same HPV type from occurring
again. However, because there are many different types of HPV,
becoming immune to one HPV type may not protect you from getting HPV
again if exposed to another HPV type.
Current partners are likely to share HPV, but this may be difficult to prove. Testing options for HPV are limited and most cases are never diagnosed.
Pap tests, for example are not specific screening for HPV; they are designed to detect abnormal cell changes of the cervix.
HPV DNA testing is not currently approved to test infection status. HPV tests are approved for clinical use with women as 1) follow-up with unclear Pap test results or 2) as primary screening for those over age 30.
Screening for men usually consists of a visual inspection to look for lesions (such as warts). Some health care providers apply an acetic wash (vinegar) as a means of highlighting lesions, but this is not a specific test for HPV and may lead to overdiagnosis.
Most cases of HPV, in either gender, remain unconfirmed
clinically.
Will I be able to transmit HPV after treatment?
Much remains unknown about HPV transmission when symptoms (lesions such as warts or cell changes) aren’t present, so experts cannot fully answer this question. However, studies show that in most cases a healthy immune system will be likely to clear, or suppress, HPV eventually. Some cases may persist for years and result in recurrent lesions, but this is not the norm. The bottom line is that most who have genital HPV DNA detected in research studies eventually test negative, often within a year or two.
Many researchers and clinicians do believe “subclinical”
HPV (virus may be in skin cells but no lesions are present) is less
likely to be transmitted than when warts or cell changes are
detected, probably due to a reduced viral load, and subsequently
think it is reasonable to say the chances of transmitting virus years
after the last clinical episode (where lesions were detected) will
become increasingly remote over time. This is not easy to prove and
the lack of a solid “yes or no” answer is frustrating.
Still, HPV does not seem likely to always be active.
Follow-up
A partner might have questions you may not be able to answer.
ASHA may be contacted by E-Mail
for help or visit their HPV
Chat Room ![]() weekdays from 5pm-6pm, ET.
weekdays from 5pm-6pm, ET.
Oral Sex Can Add to HPV Cancer Risk
The study, which appears in this week's New England Journal of Medicine (NEJM), shows that men and women who reported having six or more oral-sex partners during their lifetime had a nearly ninefold increased risk of developing cancer of the tonsils or at the base of the tongue. Of the 300 study participants, those infected with HPV were also 32 times more likely to develop this type of oral cancer than those who did not have the virus. These findings dwarf the increased risk of developing this so-called oropharyngeal cancer associated with the two major risk factors: smoking (3 times greater) or drinking (2.5 times greater). HPV infection drives cancerous growth, as it is widely understood to do in the cervix. But unlike cervical cancer, this type of oral cancer is more prevalent in men.
HPV is ubiquitous. Of the 120 strains isolated from humans — about 40 of which are in the mouth and genital tracts — Merck's recently FDA-approved vaccine, Gardasil, protects against four: HPV-6 and HPV-11, which cause warts; and HPV-16 and HPV-18, which cause about 70% of cervical cancers. Similarly, according to the study, HPV-16 was present in 72 of the 100 cancer patients enrolled in the study. Between 12,000 and 15,000 new cases of oropharyngeal cancer are diagnosed each year, and about 3,000 people die from it. "It is a significant health issue," says Dr. Robert Haddad, clinical director of the Head and Neck Oncology Program at the Dana-Farber Cancer Institute. Haddad says that public awareness of the HPV virus needs to be just like that of HIV because the virus causes multiple types of cancer.
The study's findings bring to light a part of the debate over HPV vaccination and treatment that is often overlooked: the elevated risks of cancer that being HPV-positive has for men. According to Johns Hopkins' researcher Dr. Maura Gillison, who worked on the study: "When you look at the cancers associated with HPV in men — including penile cancer, anal squamous cell carcinoma, oral cancers — it's very close to the number of cases of cervical cancer that occur in the U.S. in women every year. We need to adjust the public's perception... that only women are at risk."
In his practice, Haddad has seen an increase in the number of younger people developing this cancer, people in their 30s and 40s. He attributes it in part to a "change in sexual behavior over the last decade." He says: "The idea that oral sex is risk-free is not correct. It comes with significant risks, and developing cancer is one of them."
Gardasil has become a vaccine rock star, but vaccines to fight HPV are still in their infancy. Another study in this week's NEJM points out that while the preventative vaccine works 98% of the time to protect girls not yet infected with HPV-16 and HPV-18, the vaccine is only 17% effective against cancer precursors overall. These findings could undercut the argument ensuing in more than 15 states to make the vaccine mandatory for young girls.
Gardasil and some vaccines in clinical trial are preventative, but drug companies such as MGI Pharma are studying therapeutic vaccines to treat those already infected with the virus. "We need to come up with better vaccines — and we need to study them in men," says Haddad. Gardasil has not been tested against oral HPV, but Dr. Douglas Lowy, laboratory chief at the National Cancer Institute, says that there is every reason to think that, in principle, "the vaccine should be able to have an impact on oral cancers attributable to HPV." Lowy says that the next studies might start with a look at the rate of acquisition of oral HPV in those who are vaccinated and those who aren't.
"There's no question that the debate needs to go further than
where it is now," says Haddad. "Men are carriers and that is one way
of transmitting this virus."
Source: www.time.com/time/health/article/0,8599,1619814,00.html
![]()
Saying Yes to the HPV Vaccine - Be Cautious
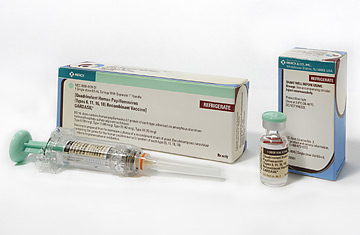
For me, the decision to take her wasn't difficult. Gardasil, which was approved by the FDA last June, protects against four strains of human papillomavirus (HPV). Two are believed to cause 70% of cervical cancer, which strikes about 11,000 U.S. women a year. The other two strains cause 90% of genital warts--so the vaccine is a twofer.
The American Academy of Pediatrics and the Centers for Disease Control and Prevention (CDC) have recommended Gardasil for girls at age 11 or 12, though it may be given any time from ages 9 through 26. The idea is to deliver protection before or not long after their "sexual debut." About 40% of girls become infected with HPV within two years of becoming sexually active. By age 50, 80% of women have had the virus at some point, though many have no symptoms, and only a small percentage of infections lead to cancer.
My pediatrician's office has been doing a brisk business in Gardasil, but a lot of parents are deeply uncomfortable with it. Texas Governor Rick Perry found that out last month when he tried to make the vaccine mandatory for girls entering sixth grade, an idea that many Texans felt contradicted the state's abstinence-only message in sex education. Since then, Merck, which makes Gardasil, has stopped lobbying states to require the vaccine for school. No other vaccine mandated for school targets a microbe that is spread mainly through sex.
To me, protecting my child from cancer outweighs any reluctance to ponder her sexual future. "But some parents are totally in denial," says my longtime pediatrician, Dr. Marc Wager of New Rochelle, N.Y. It's his practice to discuss the vaccine when parents bring a daughter for a checkup at 11 or 12. But he doesn't force it on those who resist, and he's willing to edit his discussion of HPV transmission for those who don't want a child to hear it.
Alice managed to tolerate our brief discussion of HPV without rolling her eyes. While explaining, Wager slipped in the needle--an old distraction trick that worked. "I didn't really feel it," said Alice.
"You were brave," said Wager. "Most girls say it stings more than most shots."
And it stings the wallet too. Alice will have to return for a second dose in two months and a third four months after that. The vaccine costs $120 a dose. Luckily, most private insurers are covering Gardasil, so I'll be out just $25 for each of the three visits. Kids without coverage can get the vaccine free through the federal Vaccines for Children program.
As with any new vaccine, there are plenty of unknowns about Gardasil. The CDC's Advisory Committee on Immunization Practices recently studied 542 reports on side effects out of 2.1 million doses given. Most were minor and expected: pain at the injection site, fever, dizziness and fainting. "Any procedure involving a needle has a risk of fainting," says Dr. John Iskander of the CDC's immunization safety office, which recommends waiting in the doctor's office for 15 minutes after any shot. Another unknown: how long the protection will last and whether a booster will be needed. Merck says its studies so far show that protection lasts at least five years.
My next challenge: persuading my 18-year-old daughter to go for
the shots. "Better hurry," warns Wager with a twinkle. "You'll want
to get it in before she's off to college."
Source: www.time.com/time/magazine/article/0,9171,1597467,00.html
![]()
HPV Web sites and cervical cancer prevention
Source: www.ashastd.org/hpv/hpv_learn_fastfacts.cfm
![]()
* Correction, 2/23/2007: It
had been stated that "all women who develop cervical cancer have had
a human papilloma virus (HPV) infection." According to the U.S.
National Institutes of Health, HPV infection is the primary risk
factor for cervical cancer, but other risk factors include a high
number of full-term pregnancies, use of oral contraceptives, and
smoking. This error has been corrected.
Q: How do you treat HPV warts other than
freezing or lasering them.
Is there a cream or something you can treat them with? Also, is
there a way to get rid of them?
A: Warts are noncancerous (benign) growths of skin caused by the human papilloma virus (HPV). You can develop a wart if your skin comes in contact with the virus. This can happen by touching a wart or by coming in contact with the virus indirectly, such as by walking barefoot around a swimming pool where people with warts on their feet have walked. Your skin is especially vulnerable to infection by HPV if there are cuts or abrasions on your skin.
It is difficult to get rid of a wart, especially one that has been present for a long time. Most warts will eventually go away within a few years without treatment, but the risk of spreading the infection remains until the wart is gone. There are many home remedies for treating warts. They have varying degrees of success. For example, some people have found duct tape useful; others have not. Applying one of the over-the-counter salicylic acid wart treatments is a good first step towards treating a wart yourself, but see your doctor if the warts persist.
Your doctor may prescribe topical medications such as Retin-A or prescription-strength salicylic acid preparations or may treat the wart with cryosurgery (freezing warts with liquid nitrogen). This is a very common treatment for warts. For best results, freezing the wart every two to three weeks is necessary until the wart is gone. Electrodessication (burning), curettage (scraping the wart), laser, or surgically removing can also be effective, but scarring and the return of the wart often occur.
For especially resistant warts, your doctor may use a topical application of an anti-cancer drug such as 5-Fluorouracil or inject an anti-cancer drug such as Bleomycin or interferon-alfa. Trichloroacetic acid, cantharidin (extract of the blister beetle) or other irritants may also be applied.
Imiquimod, approved by the Food and Drug Administration for the
treatment of genital warts, is an example of a new topical medication
that uses the body's own immune system to reject the wart. Your
doctor may biopsy a wart that does not respond to treatment, since
some skin cancers can resemble warts.
Safer Sex
Safer sex goes not have to mean eliminating sexual passion and
intimacy from your life. Safer sex means reducing the chance of
becoming infected. For individuals who decide to engage in sexual
intercourse, reducing the risk of infection means using latex
barriers every time you have intercourse, anal sex, fellatio or
cunnilingus.
During National Eating Disorders Awareness Week, it’s an opportunity for fathers to look at the statistics and take action to help their daughters. There are specific things fathers can do to help their daughters navigate our culture.
In their efforts to discredit the effectiveness of condoms, right-wing ideologues who want to institute sexual abstinence until marriage as a standard for all Americans have instigated an alarmist and misleading public policy and media campaign about very common, and usually benign, sexually transmitted infections — the human papilloma viruses (HPVs). State and federal legislative bills have been introduced, misinformation has been disseminated, and lawsuits have been threatened to inspire public doubt about condom use and unnecessary alarm among the many sexually active women and men — as many as three out of four — who have been infected with this extremely common, and most often harmless, infection (Cal. SB 977, 2001; Cates, 1999; "House Approves...", 2000; Leishman, 2001; Schneider & Cirmo, 2000).
While a handful of sexually transmitted HPVs can cause a variety of conditions that can lead to dangerous cancers if they remain untreated, it is a gross and dangerous exaggeration to typify HPV as a "dreaded virus" and safer-sex, public health messages advocating condom use as a "conspiracy" ("House Approves...", 2000). This fact sheet will give sexually active women and men the facts they need to understand the real nature of HPVs, what conditions HPVs cause, how those conditions can be effectively managed, and how one may reduce one's own risk of becoming infected.
Human Papilloma Virus (HPV) is a common infection that affects skin and mucous membranes, and is the cause of warts. Some types cause warts in the genital area — others cause common skin warts in other areas such as the hands or feet. Approximately 100 viral types of HPV have been identified, and about one third of these are associated with sexually transmitted genital infections (Koutsky & Kiviat, 1999). HPV has affected humans for thousands of years — ancient Greek and Roman medical records described genital lesions consistent with genital warts and associated them with sexual activity (Jay & Moscicki, 2000).
Today HPV is the most common sexually transmitted infection in the U.S. — yet 70 percent of Americans have never heard of it (Jay, 2000; KFF, 2000). Up to 20 million Americans are currently infected with sexually transmitted HPV, and it is estimated that 75 percent of reproductive age women and men have been infected with genital HPV at some point in their lives (Cates, 1999). The highest rates of genital HPV infection are found in adults between the ages of 18 and 28 (Koutsky, 1997). HPV is also prevalent among people with immunosuppressive disorders, such as HIV (Koutsky & Kiviat, 1999). HPV is believed to be widespread across racial groups and to have very little variation in prevalence across regions in the U.S. (CDC, 2000). HPV is so common, in fact, that it is considered a virtual marker for having had sex (Boonstra, 2004).
Transmission
HPV is transmitted by direct skin-to-skin contact with an infected individual. Transmission is usually from vaginal, oral, or anal sexual contact, and can occur whether or not warts or other symptoms are present (McDermott-Webster, 1999). The virus can also be transmitted from mother to infant during childbirth (Puranen, 1997). Very rarely, this "vertical" transmission is associated with development of recurrent laryngeal papillomatosis (warts on the throat) for the child — about 2,000 out of every 4 million newborns (Jay & Moscicki, 2000). This is a serious condition that may require frequent laser surgery to prevent obstruction of the infant's airways (NIAID, 2001). Some research also suggests that genital HPV can be transmitted through nonsexual routes, via fomites — inanimate objects such as towels or underwear — but more research must be conducted to examine these modes of transmission (Carson, 1997; Keller, et al., 1995; Stevens-Simon, et al., 2000).
Natural History
Although there is currently no "cure" for genital HPV infection, most cases are transient and clear themselves without medical intervention (CDC, 2001; Elfgren, et al., 2000; Ho, et al., 1998). One study designed to determine the natural history of genital HPV infection followed college women for three years (Ho, et al., 1998). HPV was detected using a sensitive DNA test that detects small amounts of HPV, even when there are no symptoms present. While there was a high rate of HPV infection (43 percent tested positive for HPV at some point over the study period), the average duration of HPV infection was eight months. Repeated HPV DNA testing showed that 70 percent of the women cleared their HPV infections within one year through the natural immune process, and only nine percent continued to be infected after two years. Another study conducted in Sweden supported these findings, with a five-year clearance rate of 92 percent (Elfgren, et al., 2000). In both studies, the viral type of HPV was a major determinant in the duration of infection, with types 16, AE7, 61, 18, and 73 having the longest average duration (Elfgren, et al., 2000; Ho, et al., 1998).
Subclinical HPV
HPV infection can be clinical (symptomatic) or subclinical (asymptomatic), and many people with HPV never know they have it (Verdon, 1997). HPV targets the deep, basal level of the skin and most often causes no clinical or microscopic changes in the cells of the skin (Keller, et al., 1995; Verdon, 1997). In some cases, subclinical HPV may cause cellular changes that are only detectable using clinical instruments or the study of cervical cells. These changes may be, in rare instances, the precursor to cancer cells (Lytwyn & Sellors, 1997).
HPV infections that cannot be seen with the naked eye may be seen with a variety of clinical tools:
During a pelvic exam, a hand lens or colposcope may be used to magnify cervical and vaginal tissue (Verdon, 1997).
Pap tests may reveal precancerous conditions of the cervix that are caused by HPV. Most often, early treatment can prevent cervical cancer (Keller, et al., 1995).
In March 1999, the U.S. Food and Drug Administration approved the Hybrid Capture II HPV test to be used as a secondary test when Pap tests are inconclusive about whether or not there have been changes in the cells of the cervix. This test uses DNA-based technology to detect 13 high-risk types of HPV (those associated with an increased risk of cancer) ("HPV DNA Tests", 2000). The Hybrid Capture II has a sensitivity of about 90 percent, meaning that it is highly likely to detect HPV in the cervix if it is present (Cuzick, 2000). Consequently, in some cases, the Hybrid Capture II can help clinicians judge a woman's risk of HPV-related cervical disease.
Genital Warts
Genital warts (condylomata acuminata) are the clinical, visible manifestation of genital HPV. In more than 90 percent of cases, they are caused by HPV types 6 and 11, which are considered low-risk types because they are not associated with increased risk of cancer (Jay & Moscicki, 2000). However, a person may be infected with more than one type of HPV at the same time.
It is estimated that one percent of the American population has genital warts, and women and men have similar rates, with a female to male ratio of 1.4:1 (Jay & Moscicki, 2000; Cockerell, 1995).
Genital warts usually start as small bumps that appear in the genital area or anus. They may be single or clusters and have a cauliflower-like appearance as they grow larger. In women, genital warts appear on the vulva, in the vagina, on the cervix, or in the anal area. In men, they appear on the foreskin, head or shaft of the penis, and in the anal area, urethra, and scrotum (Cockerell, 1995). Rarely, warts may also develop in the mouth or throat of a person who has had sexual contact with an infected person (Koutsky & Kiviat, 1999).
Genital warts usually are painless, but they may cause itching or irritation (Cockerell, 1995). Genital warts are very contagious, with an estimated rate of infection of between 30 and 60 percent from unprotected exposure (Jay & Mosicicki, 2000). The incubation period for genital warts is usually between three weeks and six months, but it may last for years after exposure (ASHA, 1998; ASHA 2000).
Treating Genital Warts
Because there is no cure for HPV infections, the purpose of treatment is to control outbreaks of warts. Some clinicians choose not to treat warts immediately in certain individuals because it has been found that in 20-to-30 percent of people, genital warts clear spontaneously within three months (Verdon, 1997; Crabb, 1997).
Genital wart treatments fall into three categories:
prescription topical chemicals designed to destroy wart tissue
surgical methods to remove wart tissue
approaches that target the underlying virus causing the wart
There are several chemicals that can be applied directly to genital warts. Some are prescribed for use at home, such as podofilox. Whenever these chemicals are used, the clinician's instructions must be followed precisely to reduce adverse side effects. Other chemical treatments include podophyllin, trichloroacetic acid (TCA), and bichloroacetic acid (BCA). Side effects of using chemicals to treat genital warts may include pain, redness, itching, burning, and swelling. Patients who are pregnant, have diabetes, are taking steroid drugs, or have poor circulation may be poor candidates for using some of these topical chemicals (Lewis, 1995).
There are several surgical methods to remove genital warts, including cryotherapy, in which individual warts are frozen off with liquid nitrogen. Another procedure is electrocautery, in which a high-frequency electric current from a wire is used to destroy the warts. Less commonly used surgical treatments include removal using scissors, scalpel, or lasers (Wright, 1998).
Least commonly used, interferon therapy is an expensive course of therapy that is designed to help the immune system target the underlying HPV infection. Interferon is a natural immune system biochemical and is injected directly into the warts. However, its effectiveness has been challenged, and it often produces side effects including flu-like symptoms (McDermott-Webster, 1999). Imiquimod is a topical treatment that a patient can apply to external genital warts at home. It stimulates the immune system to produce interferon and other immune factors to fight warts (Lamb, 2001). Imiquimod seems to produce fewer and milder side effects than other treatments (HPV Treatment and Prevention Resource, 2001).
HPV and Cancer
It is estimated that in 2004 there will be about 10,520 new cases of invasive cervical cancer in the United States, which will result in about 3,900 deaths (ACS, 2003). Worldwide, about 500,000 new cases are diagnosed each year (Shah, 1997). The median age of diagnosis for cervical cancer for all races is 48 years (Kiviat, et al., 1999).
Due largely to routine screening using Pap tests, the number of deaths attributed to cervical cancer in the United States dropped 45 percent between the periods 1972-1974 and 1992-1994, and the number of cases declined 43 percent between 1973 and 1995 (NCI, 1999a). The five-year survival rate is nearly 100 percent for pre-invasive cervical cancer, and 91 percent for early invasive cancer. The overall five-year survival rate for all stages of cervical cancer is about 70 percent (ACS, 2000).
African-Americans experience a disproportionate number of deaths from cervical cancer. The death rate is 6.7 per 100,000 for black women, compared to 2.5 per 100,000 for white women (NCI, 1999a). Latinas and Native Americans also have cervical cancer death rates that are above average (ACS, 2000).
Since the late 1800s, researchers have suspected that cervical cancer was sexually transmitted. Medical reports noted that nuns and virgins were not likely to have cervical cancer, and that women who were married to men who traveled a great deal or who had previous wives who died of cervical cancer were more likely to develop cervical cancer ("The Cervical Cancer Virus," 1995). Today, certain types of HPV have been established as causal agents in the development of the cellular changes that may lead to cervical cancer (Janicek & Averette, 2001). Large studies have found that HPV is present in more than 93 percent of cervical cancer tumors (NCIa). HPV 16 is responsible for about 50 percent of cervical cancers. HPV 18, 31, and 45 account for another 30 percent of cases. Other HPV types are associated with the remaining 20 percent of cases (Shah, 1997).
Even though HPV is considered a cause of cervical cancer, only one out of 1,000 women with HPV develops invasive cervical cancer (ACOG, 2000). Most HPV infection never leads to the development of cervical cancer — even in the absence of medical intervention — and treating precancerous cervical lesions detected by Pap tests has greatly reduced the rate of invasive cervical cancer (Ho, et al., 1998; NCI, 1999a).
HPV appears to be necessary, but not sufficient, to the development of cervical cancer. Besides HPV type, researchers believe there are several cofactors that may contribute to the development of cervical cancer. These may include smoking, HIV infection, diet, hormonal factors, and the presence of other sexually transmitted infections, such as chlamydia and/or herpes simplex virus 2 (Anttila, et al., 2001; CDC, 1999; NCI, 1999b).
Certain types of genital HPV are also now considered to be a cause of most cancers of the vagina, vulva, anus, and penis. Although each of these cancers occurs less frequently than does cervical cancer, taken together they equal nearly half the number of cases of cervical cancer in the U.S. (Eng & Butler, 1997). The average age for diagnosis of these cancers is significantly later than for cervical cancer. The median age of diagnosis for vaginal cancer is 67 years and 70 years for vulvar cancer. Anal cancer is typically diagnosed at 66 years of age for women and 63 years for men, and the average age of diagnosis for cancer of the penis is 66 years (Kiviat, et al., 1999). As is the case with cervical cancer, HPV 16 and HPV 18 are most often associated with vaginal, vulvar, anal, and penile cancers (Eng & Butler, 1997). An association has also been made between HPV and oral, head, and neck cancers, although further research needs to be conducted to establish a causal relationship (Mork, et al., 2001; Schwartz, et al., 1998). Men are three times more likely than women to develop head and neck cancers (HPV Treatment and Prevention Resource, 2001).
Prevention
Abstinence or lifelong monogamy are the most effective ways to avoid HPV infection. However, for most sexually active women, the most important preventive measure women can take to protect themselves from developing cervical cancer is having regular Pap tests (Janicek & Averette, 2001). Avoiding skin-to-skin contact with someone with HPV is the most effective strategy to prevent HPV infection. And although condoms may not eliminate the risk of transmitting HPV, the CDC recommends them for risk reduction (CDC, 2001). Since HPV may shed beyond the covered area, however, condoms do not provide as complete protection as they do for some other pathogens, such as HIV and gonorrhea (Stone, et al., 1999). The claims of condom-use opponents who suggest that condom use leads to increased numbers of HPV infections are false and alarmist. Condom use cannot be blamed for the high prevalence of HPV infection or the incidence of cervical cancer among women in the U.S.
Vaccines against HPV are currently being developed but are still years away from being available (HPV Treatment and Prevention Resource, 2001). Both prophylactic vaccines that prevent HPV infection (most vaccines being developed target HPV 16) and therapeutic vaccines designed to prevent the development of precancerous cells are being developed. Other vaccines in development are both prophylactic and therapeutic in nature (Austell, 2000).
While HPV is endemic among sexually active women and men in the U.S., it is reassuring to know that these infections most often remain asymptomatic and symptoms, if they occur, are usually manageable. Equally reassuring is the fact that condom use is likely to reduce the risk of infection. To reduce the risk of developing the most dangerous conditions associated with HPVs, women and men who are sexually active should have periodic physical checkups including evaluation of any symptoms of sexually transmitted infections. Sexually active women should be sure to have routine Pap tests as well.
Additional Resources
American Social Health Association (ASHA)
P.O. Box 13827
Research Triangle Park, NC 27709
(919) 361-8400
(919) 361-8425 (fax)
www.ashastd.org
American Cancer Society (ACS)
1599 Clifton Rd. NE
Atlanta, GA 30329
800-ACS-2345
(404) 329-7530
www.cancer.org
National Center for HIV, STD, & TB Prevention
Centers for Disease Control and Prevention
Atlanta, GA 30333
nchstp@cdc.gov
www.cdc.gov/nchstp/od/nchstp.html
Toll-free voice information: 888-232-3228
CDC STI Hotline: 800-227-8922
Cited References
ACS — American Cancer Society. (2003, accessed 2004, January 22). [Online]. http://www.cancer.org/docroot/CRI/CRI_2_1x.asp?rnav=criov&dt=8
ACOG — American College of Obstetricians and Gynecologists. (2000, accessed 2001, May 23). "Make Decisions about Human Papillomavirus Based on Sound Medicine, Rather than Politics." [Online.] http://www.acog.org/from_home/departments/dept_notice.cfm?recno=11&bulletin=1083
Anttila, Tarja, et al. (2001). "Serotypes of Chlamydia Trachomatis and Risk for Development of Cervical Squamous Cell Carcinoma." The Journal of the American Medical Association, 285(1), 47-51.
ASHA — American Social Health Association. (1998). HPV in Perspective.
_____. (2000, accessed 2001, May 23). HPV: Get the Facts External Genital Warts. [Online]. http://www.ashastd.org/hpvccrc/gw.html
Austell, Amy, ed. (2000, Winter). "The Vaccine Marathon." HPV News, 10, 1-5.
Boonstra, Heather. (2004). "Comprehensive Approach Needed to Combat Sexually Transmitted Infections Among Youth." The Guttmacher Report on Public Policy, 7(1), 3-4, 13.
California SB 977. (2001). Condom Warning Labels.
Carson, Sylvia. (1997). "Human Papillomatous Virus Infection Update: Impact on Women's Health." The Nurse Practitioner, 22(4), 24-37.
Cates, Willard. (1999). "Estimates of the Incidence and Prevalence of Sexually Transmitted Diseases in the United States." Sexually Transmitted Diseases, 26(4), s2-s7.
CDC — Centers for Disease Control and Prevention. (1999, accessed 1999, October 1). STD Trends. [Online]. http://www.cdc.gov/nchstp/dstd/Stats_Trends/STD_Trends/
_____. (2000, accessed 2001, January 25). Tracking the Hidden Epidemic: Trends in STDs in the United States, 2000 [Online]. http://www.cdc.gov/nchstp/dstd/Stats_Trends/Trends2000.pdf
_____. (2001, accessed May 25). Genital HPV Infection. [Online]. http://www.cdc.gov/nchstp/dstd/Fact_Sheets/FactsHPV.htm
"The Cervical Cancer Virus." (1995). Discover, 16, 24-26.
Cockerell, Clay. (1995). "Human Papillomavirus Infections." Journal of the International Association of Physicians in AIDS Care, 1(9), 32-36.
Crabb, Kenneth. (1997, accessed May 5, 2001). "Anogenital Human Papillomavirus Infection." The Medical Journal of Allina, 6(3). [Online]. http://www.allina.com/Allina_Journal/Summer1997.crabb.html
Cuzick, Jack. (2000, January 5). "Human Papillomavirus Testing for Primary Screening." Journal of the American Medical Association, 283(1), 108-109.
Elfgren, Kristina, et al. (2000). "A Population-Based Five-Year Follow-Up Study of Cervical Human Papillomavirus Infection." American Journal of Obstetrics and Gynecology, 183(3), 561-567.
Eng, Thomas & William Butler, eds. (1997). The Hidden Epidemic: Confronting Sexually Transmitted Diseases. Washington, DC: National Academy Press.
Ho, Gloria, et al. (1998). "Natural History of Cervicovaginal Papillomavirus Infection in Young Women." New England Journal of Medicine, 338(7), 423-428.
"House Approves Labeling Condoms with Warnings about HPV Infection." (2000, May 26). AIDS Policy and Law, 15(1).
"HPV DNA Tests: Studies Target Use for Cancer Screening." (2000, May). STD Quarterly, 1-3.
HPV Treatment and Prevention Resource: New Opportunities, New Challenges. (2001). Decatur, GA: Flynn Publications.
Janicek, Mike & Averette, Hervy. (2001). "Cervical Cancer: Prevention, Diagnosis, and Therapeutics." CA: A Cancer Journal for Clinicians, 51(2), 92-114.
Jay, Naomi & Moscicki, Anna-Barbara. (2000). "Human Papilloma Virus Infection in Women." In: Marlene Goldman & Maureen Hatch, eds. Women & Health. San Diego, CA: Academic Press.
KFF — Kaiser Family Foundation. (2000, accessed 2001, May 23). National Survey of Public Knowledge of HPV, the Human Papillomavirus. [Online.] http://www.kff.org/content/2000/20000217a/HPVChartpack2.PDF
Keller, Mary, Egan, Judith, & Mims, L. Fern. (1995). "Genital Human Papillomavirus Infection: Common but not Trivial. " Health Care for Women International, 16, 351-364.
Kiviat, Nancy, et al. (1999). "Cervical Neoplasia and Other STD-Related Genital Tract Neoplasias." In: King Holmes, et al., eds. Sexually Transmitted Diseases, 3rd ed. New York: McGraw-Hill
Koutsky, Laura & Kiviat, Nancy. (1999). "Genital Human Papillomavirus." In: King Holmes, et al., eds. Sexually Transmitted Diseases, 3rd ed. New York: McGraw-Hill
Koutsky, Laura. (1997). "Epidemiology of Genital Human Papillomavirus Infection." The American Journal of Medicine, 102(5A), 3-8.
Leishman, Katie. (2001, July 27). "Controversy and Need for Study on Condoms." United Press International.
Lamb, Steven. (2001, accessed May 20). Imiquimod. [Online]. http://www.dermnet.org.nz/dna.imiquimod/info.html
Lewis, Ricki. (1995). "New Choices for Coping with Genital Warts." FDA Consumer, 29(4), 17-21.
Lytwyn, Alice & Sellors, John. (1997). "Sexually Transmitted Human Papillomaviruses: Current Concepts and Control Issues." The Canadian Journal of Human Sexuality, 6(2), 113-126.
McDermott-Webster, Marian. (1999). "The HPV Epidemic." American Journal of Nursing, 99, 24L-24N.
Mork, Jon, et al. (2001). "Human Papillomavirus Infection as a Risk Factor for Squamous-Cell Carcinoma of the Head and Neck." New England Journal of Medicine, 344(15), 1125-1131.
NCI — National Cancer Institute. (1999a, accessed 2001, May 21). Cervical Cancer: Backgrounder. [Online]. http://rex.nci.nih.gov/massmedia/backgrounders/cervical.html
_____. (1999b, accessed November 9). Prevention of Cervical Cancer. [Online]. http://imsdd.med.uni-bonn.de/cancernet/304734.html
NIAID — National Institute of Allergy and Infectious Diseases. National Institutes of Health. Public Health Service. (2001, accessed May 23). Human Papillomavirus and Genital Warts. [Online]. http://www.niaid.nih.gov/factsheets/stdhpv.htm
Puranen, Mirja, et al. (1997). "Exposure of an Infant to Cervical Human Papillomavirus Infection of the Mother is Common." American Journal of Obstetrics and Gynecology, 176(5), 1039-1045.
Schneider, Yvette & Cirmo, Heather. (2000, accessed October 31, 2001). Rampant STD Virus Not Getting Sufficient Attention. [Online]. http://www.frc.org/get/ar00h9.cfm?CFID=121780&CFTOKEN=46584315
Schwartz, Stephen, et al. (1998, November 4). "Oral Cancer Risk in Relation to Sexual History and Evidence of Human Papillomavirus Infection." Journal of the National Cancer Institute, 90(21), 1626-1636
Shah, Keerti V. (1997). "Human Papillomaviruses and Anogential Cancers." The New England Journal of Medicine, 337(19), 1386-1388.
Stevens-Simon, Catherine, et al. (2000). "The Prevalence of Genital Human Papillomavirus Infections in Abused and Nonabused Preadolescent Girls." Pediatrics, 106(4), 645-649.
Stone, Katherine, et al., (1999). "Barrier Methods for the Prevention of Sexually Transmitted Diseases." In King Holmes, et al., eds. Sexually Transmitted Diseases, 3rd ed. New York: McGraw-Hill.
Verdon, Mary. (1997). "Issues in the Management of Human Papillomavirus Genital Disease." American Family Physician, 55, 1813-1820.
Wright, Tracy. (1998). "Genital Warts: Their Etiology and Treatment." Nursing Times, 94, 52-54.
the Katharine Dexter McCormick Library
Planned Parenthood affiliate health centers provide culturally competent, high quality, affordable health care to millions of diverse women, men, and teens every year. Planned Parenthood welcomes everyone — regardless of race, age, disability, sexual orientation, or income.
These documents are for informational purposes only and are not intended to constitute medical advice, diagnosis, or treatment.
For medical questions, or to schedule an appointment with the nearest Planned Parenthood health center, call toll-free 1-800-230-PLAN
or 1-800-230-7526
Source: Planned Parenthood® Federation of America, Inc., www.plannedparenthood.org/pp2/portal/files/portal/medicalinfo/sti/fact-HPV-virus.xml
|
|